12 million Americans suffer a diagnostic error every year, and up to one-third of these suffer serious permanent harms, including disability or death.” (3)
Unfortunately, when a serious medical diagnosis is missed, it can result in even more pain and suffering for a patient than if the illness was identified correctly. According to researchers, “delayed cancer diagnosis is believed to be one of the most harmful and costly types of diagnostic error.”(2)
According to the best numbers available, “12 million Americans suffer a diagnostic error every year, and up to one-third of these suffer serious permanent harms, including disability or death.”(3)
What Is a Misdiagnosis?
A misdiagnosis or diagnostic error may mean you have been diagnosed with cancer when you don’t have cancer or that you have cancer that has not been diagnosed.
According to one medical expert, “The Institute of Medicine defines diagnostic error as ‘the failure to establish an accurate and timely explanation of the patient’s health problem(s) or communicate that explanation to the patient.”(4)
As he explains it, “Misdiagnosis is incredibly frequent because medicine is incredibly hard. There’s uncertainty and complexity and incomplete information all the time.”(5)
If you are the victim of a diagnostic error, you could benefit from the experience and knowledge of a cancer misdiagnosis attorney.
How Can a Cancer Misdiagnosis Attorney Help?
A knowledgeable and experienced cancer misdiagnosis attorney evaluates your situation to determine if there are grounds for a cancer misdiagnosis lawsuit to gain compensation for you or your loved ones.
The attorney considers factors such as:
- Did the doctor provide the professional standard of care?
- Was the outcome of the misdiagnosis avoidable?
- Did the misdiagnosis result in economic and noneconomic damage, including pain and suffering?
Not every situation is clear-cut, and seeking compensation requires familiarity with the law. That’s why you need an attorney who has dealt with these types of cases before.
Was My Doctor’s Mistake Malpractice?
Medicine is complicated, and mistakes do happen. However, not every mistake equates to medical malpractice.
Doctors are responsible for providing the care that any reasonable doctor would provide under the same or similar circumstances.
To prove medical malpractice, a trained cancer misdiagnosis attorney identifies instances where a doctor may have made an unreasonable mistake and should be held accountable.
For a doctor to be found liable, there must be a breach of the professional standard of care as well as the patient suffering from some injury.
The injury must be one that would not have happened if the doctor did not breach the professional standard of care.

Cancer Misdiagnosis Lawsuits
As a national law firm, Weitz & Luxenberg P.C. has been winning cases for clients for 30 years.
Our attorneys are highly trained and experienced with cancer misdiagnosis lawsuits. Our firm has the resources to take on large, complex, and lengthy litigations, especially for those who would otherwise be without a voice.
Additionally, an important component in any cancer misdiagnosis lawsuit is the pain and suffering the plaintiff endured because of the cancer misdiagnosis. This includes undergoing unnecessary surgeries, radiation, or chemotherapy treatments. It also includes any financial burden the plaintiff has incurred due to the misdiagnosis.
W&L Holds Doctors Liable
When you work with W&L you get a team of attorneys that is willing to challenge the medical professional and institutions that caused you harm. We have been successful in our compensation fights for many clients.
For example, attorneys at W&L successfully negotiated a substantial financial settlement for Joan S., who lost her husband, Albert, to colon cancer in 2009. Albert’s death was unnecessary; his cancer was very treatable at the time it was detected. But he didn’t know.
Doctors failed to tell Albert he had colon cancer, although they had detected it 18 months before his death — in plenty of time to treat it. Albert’s doctors never even ordered any treatment for his colon cancer.
Have you experienced pain and suffering from your cancer being misdiagnosed? Contact us now for a free consultation.
Get a Free Case ReviewJoan S. says, “My lawsuit was not just about resolution and restitution. It was also about retribution. I wanted the people who were responsible for Albert’s death to be punished. The way that would happen is if they had to pay a steep price for what they did.”
The likelihood of survival is an important consideration in the doctor’s liability, as is the plaintiff’s reduced quality of life. Additionally, any “lost chance” at treatment or survival is taken into account.
W&L Champions Victims & Their Families
In another cancer misdiagnosis lawsuit, Weitz & Luxenberg negotiated a $1.975 million settlement on behalf of the estate of a 51-year-old woman who died.
Lynette Ryan died from a ruptured pancreas that was misdiagnosed. The first diagnosis was gastritis, then carcinomatosis — a type of metastasized cancer, and finally ovarian cancer. An autopsy finally determined the true cause of Lynette’s death was a ruptured appendix.
Gary Klein, the W&L managing attorney, said, “You can only get these substantial settlements if you choose a law firm with the experience to go the distance. Your legal counsel has to know how to handle your needs, and balance the legal aspects with a need for compassion and understanding, in order to have a successful lawsuit.
What to Know About Misdiagnosed Cancers
A sense of compassion is essential when dealing with our clients who get a cancer misdiagnosis. Sadly, such cases are not confined to one form of the disease.
Many cancers are potentially life-threatening, so early detection and intervention is key. When cancer is misdiagnosed, the chances for a positive outcome are jeopardized.
Even when a doctor’s cancer diagnosis turns out to be incorrect, it may not be medical malpractice. Some cancers are very hard to detect, or benign conditions might reasonably be mistaken as malignant.
Testimony from additional medical experts is required to determine if a doctor has provided the reasonable standard of care in your particular case.
Modern cancer treatments have greatly increased survival and recovery rates among cancer patients. So be aware that a misdiagnosis does not have to be fatal for a cancer misdiagnosis lawsuit to be successful.
If you have been diagnosed with cancer, but in fact do not have cancer, you may be entitled to compensation for unnecessary surgeries or treatments.
Many states also allow you to be compensated for living under threat of a cancer misdiagnosis and the fear and anguish you suffer due to misdiagnosis.
Medical malpractice cases are highly complex, with every case being unique; success depends upon the circumstances of each.
A trained and experienced cancer misdiagnosis attorney can help you determine the potential for success of your case.
What Is Cancer?
According to the National Cancer Institute at the National Institutes of Health, “Cancer is the name given to a collection of related diseases. In all types of cancer, some of the body’s cells begin to divide without stopping and spread into surrounding tissues.”(6)
In a healthy person, cells divide to form new cells as they are needed. As this happens, old and damaged cells die off and are replaced by new ones. In cancer, this process breaks down.(7)
In someone who has cancer, “old or damaged cells survive when they should die, and new cells form when they are not needed. These extra cells can divide without stopping and may form growths called tumors.”(8)
The cancers form into solid tumors, which become masses of tissue. Tumors can spread and invade other nearby tissues in the body.(9) Tumors are classified as either benign or malignant.
Experiencing pain and suffering after your cancer was misdiagnosed? Speak to a top attorney for a free consultation.
(917) LAWYERSWhile a benign tumor can grow large, the cells from this type of tumor do not break off and travel to other parts of the body. And, once the tumor is removed, it generally does not grow back.(10)
Such is not the case with malignant tumors. Malignant tumor cells break off and spread to other areas of the body, forming new tumors.(11)
What Causes Cancer?
The causes of cancer are not fully understood. The American Cancer Society suggests there are a variety of factors at play in the development of cancer, from genetics to diet and exercise, from exposure to viruses and carcinogens to radiation and chemicals. Even microwaves and cell phones have been listed among the possible causes.(12)
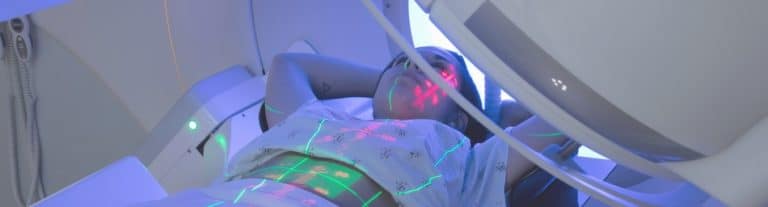
How Is Cancer Diagnosed?
To diagnose cancer, doctors first conduct a physical exam during which they ask questions about your personal medical history as well as the medical history of your family members.
Next, doctors may conduct tests to aid in the diagnostic process. Common tests used to diagnose cancer include lab tests where samples of blood, urine, and other bodily fluids are taken for measurement. Biopsies — procedures where tissue samples are extracted to be viewed under a microscope — may also be performed. Additionally, imaging procedures might be utilized.(13)
According to the National Cancer Institute, imaging procedures help doctors see if there are tumors present in the body. Imaging technologies include:
- CT scans: X-rays of organs and other tissues in the body.
- Nuclear scans: pictures obtained when a small amount of radioactive material is injected into the body as a tracer.
- Ultrasounds: images gathered from sound waves when they bounce off tissues in the body, like an echo. The picture is called a sonogram.
- MRIs: images obtained from strong magnets linked to a computer.
- PET scans: 3-D images of organs and tissues showing how they are working.(14)
An error anywhere in the diagnostic process, whether made by the doctors or the technologies used, can result in a cancer misdiagnosis.
Blood & Laboratory Tests Pitfalls
As a rule, blood tests and other laboratory tests are the first tools employed by physicians in making a diagnosis.
While these tests provide much needed information, which may be indicative of cancer, they are rarely relied upon as the sole basis for forming a cancer diagnosis.
Even when blood-born cancers are in question, other tests may be necessary to confirm a diagnosis of leukemia, lymphoma, or myeloma.
Blood and lab tests are usually followed up with biopsies of the organs or tissues in question.
Biopsy Issues
Biopsies are the removal of tiny pieces of bodily tissues for examination under a microscope by a type of doctor called a pathologist. Newer techniques, such as needle aspiration, have even further reduced the size of the tissue sample necessary for the procedure.
Upon viewing the cells in the tissue sample, the pathologist determines if they are benign (not harmful) or malignant (cancerous). The difference between benign and malignant cells can be subtle, adding a layer of difficulty to the process.
Adding yet another layer of difficulty, the pathologists must also determine the degree of malignancy in any malignant cells present in the tissue sample.
It is this level of difficulty, which depends greatly on a pathologist’s abilities, that increases the chances of a misdiagnosis.
Commonly misdiagnosed cancers include:
- Breast cancer
- Cervical cancer
- Kidney cancer
- Lung cancer
- Ovarian cancer
- Pancreatic cancer
Breast Cancer Misdiagnosis
While it is true that early detection and intervention are critical to survival of breast cancer, there are indications that women within certain age groups might be susceptible to misdiagnosis.
Over a 3-year period, 7004 patients were discharged with a nonmalignant diagnosis. Twenty-nine patients were subsequently diagnosed with breast cancer over the next 36 months.” (16)
A 2009 study, One-stop diagnostic breast clinics: how often are breast cancers missed?, was undertaken to “Estimate the number of patients discharged… who subsequently develop breast cancer and to determine how many of these cancers had been ‘missed’ at initial assessment.”(15)
“Over a 3-year period, 7004 patients were discharged with a nonmalignant diagnosis. Twenty-nine patients were subsequently diagnosed with breast cancer over the next 36 months.”(16)
The study reported, “The lowest sensitivity of initial assessment was seen in patients of 40-49 years of age, and these patients present the greatest imaging and diagnostic challenge.”(17)
Cervical Cancer Misdiagnosis
Key to the diagnosis and treatment of cervical cancer is the use of imaging technologies like CT scans, MRIs, and PET scans. These imaging technologies depend on contrast resolution.(18)
Errors can arise from poor contrast resolution of a tumor and tissues, calling into question their reliability and potentially leading to cervical cancer misdiagnosis.
Also, other problematic issues for imaging technologies are limitations on the field of view, alterations in signal intensity, metabolic activity of a tumor, and the presence of brown fat.(19)
Kidney Cancer Misdiagnosis
The most common form of kidney cancer in adults is renal cell carcinoma. And in the past, biopsies have not always proven effective in the diagnosis of kidney cancer.
While a 2016 study by Fox Chase Cancer Center on the use of biopsies for kidney cancer diagnosis suggests that core-needle biopsies improve effectiveness, researchers acknowledge important limitations to biopsies.
In the study, “biopsies led to inaccurate classifications of tumor grade in 37 percent of surgical cases, putting patients at risk of under-treatment.”(20)
“In addition, 30 percent of patients who had biopsies and underwent surgery potentially had low-risk tumors, suggesting that they may have been over-treated and better managed by active surveillance.”(21)
Lung Cancer Misdiagnosis
In a 2017 article published in Diagnostic and Interventional Radiology, the authors note that “Lung cancer accounts for 1.59 million deaths per year worldwide.”(22)
They also note that, “In 90% of the cases, errors in diagnosis of lung cancer occur on chest radiographs.”(23)
Among the reasons for overlooking pulmonary malignancy are:
- Observer error in scanning, recognition, or decision-making
- Specific characteristics of the undetected lesion related to size, conspicuity, and location
- Technical inaccuracies involving image quality and patient positioning or movement.(24)

Ovarian Cancer Misdiagnosis
According to the American Cancer Society, “Ovarian cancer ranks fifth in cancer deaths among women, accounting for more deaths than any other cancer of the female reproductive system.”(25)
Roughly half of the women diagnosed with ovarian cancer are 63 years of age and up.(26)
Testing for ovarian cancer typically includes a colonoscopy and laparoscopy. Doctors do these tests in order to look at the colon and rectum, which helps diagnose the disease and determine that it has not spread.
The colonoscopy, as with other imaging technologies, relies on the use of contrast resolution to view the colon and rectum. Therefore, the potential for contrast resolution errors exists and can lead to misdiagnosis.
A laparoscopy is the insertion of a lighted tube into the body to view the abdomen and pelvic cavity and to perform a biopsy. The potential for misdiagnosis stems from instrument failure or incorrect use.
Pancreatic Cancer Misdiagnosis
Frequently, the size of the pancreas has been viewed as indicative of pancreatic cancer, but this is not always the case. If doctors are not alert, a misdiagnosis may result.
It has long been known that the liver can be invaded by fat cells, particularly if the patient has Type 2 diabetes or pancreatitis. Both conditions may cause a fatty liver.
But the fat cells can also invade the pancreas. Authors of a 2015 case report determined that an “Enlarged pancreas is not always a cancer, but pancreatic steatosis is characterized by pancreatic enlargement.”(27)
The authors reported that when a non-obese female was diagnosed with a mass in the pancreas, “Magnetic resonance imaging (MRI) was carried out to define the characteristics of the pancreatic mass. MRI confirmed the diagnosis of fat pancreas.”(28)
